 Contributor: Rachael Mattice is the Content Manager for Sovereign Health Group, an addiction, mental health and dual diagnosis treatment provider. Rachael received her bachelor’s degree in journalism and mass communication from Purdue University.
Contributor: Rachael Mattice is the Content Manager for Sovereign Health Group, an addiction, mental health and dual diagnosis treatment provider. Rachael received her bachelor’s degree in journalism and mass communication from Purdue University.
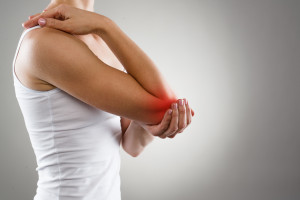
Fibromyalgia is the most common cause of widespread musculoskeletal pain1 , affecting more than 6 million patients in the United States.
This syndrome is associated with significant clinical and economic burden to patients, the health care system, and society as a whole. Fibromyalgia is a relatively new diagnosis, and the first studies were published in the early 1990s.
Fibromyalgia is a controversial issue.
Many clinicians still do not believe it is a true diagnosis and instead label these patients’ pain as “purely psychological.”
However, fibromyalgia has been accepted as a legitimate clinical entity by many well-respected organizations, such as the American Medical Association (AMA), the National Institutes of Health (NIH), and the World Health Organization (WHO).
According to a Medscape article on fibromyalgia2 , “the typical fibromyalgia patient has seen an average of 15 physicians and has had the condition for approximately five years before receiving a correct diagnosis.
More than 50 percent of cases are misdiagnosed, and many patients undergo unnecessary surgery, endure costly treatments that provide little benefit” or get hooked on pain medication.
What is Fibromyalgia?
Fibromyalgia is a chronic pain and type of clinical fatigue syndrome comprising multiple pain and tenderness points in the body and is generally seen in middle-aged females.
 To receive a fibromyalgia diagnosis, one must have pain and tenderness along multiple joints on both sides of the body for at least three months, as well as fatigue, stiffness, cognitive difficulties, and anxiety or depression.
To receive a fibromyalgia diagnosis, one must have pain and tenderness along multiple joints on both sides of the body for at least three months, as well as fatigue, stiffness, cognitive difficulties, and anxiety or depression.
There are a standard 18 fibromyalgia tender points throughout the body that include the forehead, back of the neck, muscles in the upper back, the ribs, the gluteal region, the upper leg region, elbows, knees, and fingers.
No Clear Answer
The actual reason why fibromyalgia occurs is not fully understood. However, researchers do know that fibromyalgia is a disorder of central nervous system pain processing3 in which patients have a lower threshold of pain and of other stimuli, such as heat, noise and strong odors.
“Brain scans of patients with fibromyalgia showed that they processed nonpainful stimuli, such as sound and touch, differently than the brains of people without the disorder. This may explain why patients often complain of hypersensitivity to sensations in everyday life,” according to Medscape Medical News4 .
Most people who live with chronic pain also suffer from depression; patients with fibromyalgia are no different. In fact, negative emotions, such as anger and sadness, have been shown to be direct amplifiers of pain in women with and without fibromyalgia5 .
Narcotic Overuse in Fibromyalgia
No specific cure exists for fibromyalgia. However, education, lifestyle changes including regular physical activity, and proper medications can help individuals regain control and achieve significant improvement in their daily lives.
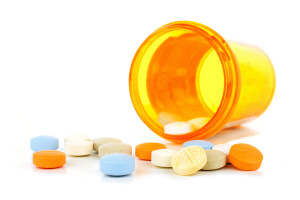 As in any pain disorder, fibromyalgia patients often turn to narcotic pain medications to treat the pain, even though narcotics (opioids) have no proven benefits for patients with this disease.
As in any pain disorder, fibromyalgia patients often turn to narcotic pain medications to treat the pain, even though narcotics (opioids) have no proven benefits for patients with this disease.
Recent evidence shows that more than four-fifths of fibromyalgia patients receive opioid therapy6 , and ironically opioid medications have no evidence of treatment and also have a high potential for abuse. Examples of these popular opioids are hydrocodone and oxycodone.
Narcotic Addictions
Narcotics also known as opioids are naturally addicting substances because they produce the sense of euphoria and pain relief; however, they also can cause respiratory depression, constipation, drowsiness, dizziness and many other negative side effects.
Over time, patients will develop a tolerance to these prescription pain medications and will eventually become dependent on narcotics, causing withdrawal symptoms if these medications are abruptly decreased or stopped.
Addiction to pain medications is a common fear that most patients and physicians share, because becoming addicted can severely change patients’ entire lives and have negative effects on their personal, professional and social lives.
Why Narcotics do not Treat Fibromyalgia
The human body naturally produces pain relieving chemicals called opioids. In fibromyalgia patients, altered natural opioid activity occurs in the central nervous system, which further complicates the use of prescription pain medications.
 A study utilizing positron emission tomography (PET) found that patients with fibromyalgia had decreased mu opioid receptor availability in areas of the brain that are responsible for pain perception.
A study utilizing positron emission tomography (PET) found that patients with fibromyalgia had decreased mu opioid receptor availability in areas of the brain that are responsible for pain perception.
Natural opioid levels are actually increased in fibromyalgia patients, which could be the cause for the decrease in opioid receptor availability, decreasing the effectiveness of these narcotics in fibromyalgia patients (Harris RE, Clauw DJ, Scott DJ, et al. Decreased central mu-opioid receptor availability in fibromyalgia. J Neurosci. 2007;27:10000–10006).
Effective Fibromyalgia Treatments
Only three medications -- duloxetine, milnacipran and pregabalin -- are approved by the U.S. Food and Drug Administration for fibromyalgia treatment . However, some antidepressants such as amitriptyline and fluoxetine are used off-label to treat fibromyalgia and have been shown to have positive outcomes.
As with all musculoskeletal illnesses, exercise, cognitive behavioral therapy, a healthy diet, acupuncture, and stress-relieving therapies such as meditation have been used to treat fibromyalgia pain and chronic fatigue symptoms. Although this is a complicated and controversial disease, it is important for clinicians and patients to be aware that opioids should not be used for pain relief.
Community Discussion – Share your thoughts here!
What has been your experience with fibromyalgia and avoiding opioids in treatment?
About the Author:
Rachael Mattice is the Content Manager for Sovereign Health Group, an addiction, mental health and dual diagnosis treatment provider. Rachael is a creative and versatile journalist and digital marketing specialist with an extensive writing and editing background.
Her portfolio includes numerous quality articles on various topics published in print and digital formats at award-winning publications and websites. To learn more about Sovereign Health Group’s mental health treatment programs and read patient reviews, visit http://www.sovhealth.com/. Follow Sovereign Health Group on Twitter, Facebook, Google+ and LinkedIn.
The opinions and views of our guest contributors are shared to provide a broad perspective of addiction. These are not necessarily the views of Addiction Hope, but an effort to offer discussion of various issues by different concerned individuals.
Last Updated & Reviewed By: Jacquelyn Ekern, MS, LPC on May 6th, 2015
Published on AddictionHope.com
