 Contributor: Rachael Mattice is the Content Manager for Sovereign Health Group, an addiction, mental health and dual diagnosis treatment provider. Rachael received her bachelor’s degree in journalism and mass communication from Purdue University.
Contributor: Rachael Mattice is the Content Manager for Sovereign Health Group, an addiction, mental health and dual diagnosis treatment provider. Rachael received her bachelor’s degree in journalism and mass communication from Purdue University.
What Is Sickle Cell
Sickle cell pain crisis is one of the most excruciating pain episodes a child can have. These episodes continue throughout childhood into adulthood, leading to a lifetime of pain. Sickle cell disease affects children around the world. Originating in West Africa, the disease has the highest prevalence in African and Middle Eastern populations.
Sickle cell disease manifests very early in life. Universal screening for the disease is mandatory in the U.S. at birth in every infant. For the first 6 months of life, the mother’s blood protects the infant and, therefore, children will not be asymptomatic until after 6 months of age.
A Genetic Disorder
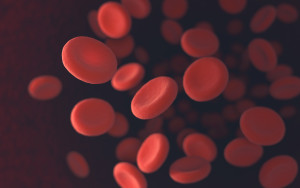
Sickle cell disease is a genetic disorder resulting from the presence of mutated hemoglobin, a carrier molecule in blood that helps delivers oxygen to tissues in the body.
It results in a type of anemia that breaks down the blood molecules, known as “sickling,” because of the abnormal shape of the hemoglobin molecules. This results in decreased oxygen delivery to the bones, known as bone infarction, causing extreme pain in bony areas of the body, such as the spine, legs and arms.
The Statistics
Sickle cell pain crisis, often called vaso-occlusive crisis, is the most common manifestation of sickle cell disease in children. Vaso-occlusive crisis results when a change in altitude or temperature occurs, and is more prevalent in cases of dehydration, infection, pregnancy, alcohol intoxication and emotional stress. Approximately half the individuals with sickle cell disease will experience vaso-occlusive crises.
 The crises frequency varies immensely. Some individuals have as many as six or more episodes annually, whereas others might only have episodes at great intervals or none at all.
The crises frequency varies immensely. Some individuals have as many as six or more episodes annually, whereas others might only have episodes at great intervals or none at all.
According to the Centers for Disease Control and Prevention1 and the National Institutes of Health2 , sickle cell anemia is the most common inherited blood disorder in the United States, more than 70,000 people in the U.S. have sickle cell disease, and the disease occurs in 1 in every 500 African Americans.
Treatments
The pain episode is the most distressing symptom in patients with sickle cell disease. Pain crises begin suddenly and the crisis might last several hours to several days and terminate as abruptly as it began.
Pain can be severe and debilitating, and it often interferes with school performance or employment. Vaso-occlusive crisis and chronic pain are associated with considerable economic loss and disability.
The Struggle
Repeated episodes of lack of oxygen delivery to joints, bones, and growth plates result in the breakdown and death of these areas, especially in weight bearing areas such as the femur. This complication is associated with chronic pain and disability, and might require changes in employment and lifestyle.
Anti-inflammatory medications, such as ibuprofen and Toradol, along with high-dose narcotics, such as morphine, Dilaudid and Percocet, are given to relieve the pain. Patient-controlled analgesia (PCA) pumps are commonly used to treat the pain crisis brought on by sickle cell disease.
 The child can press the PCA pump to release a narcotic pain medicine when the pain becomes excruciating. There is a maximum amount of analgesic that can be released in an hour to prevent the child from overdosing on narcotics. As the pain begins to subside, the child is slowly weaned off narcotic medications.
The child can press the PCA pump to release a narcotic pain medicine when the pain becomes excruciating. There is a maximum amount of analgesic that can be released in an hour to prevent the child from overdosing on narcotics. As the pain begins to subside, the child is slowly weaned off narcotic medications.
Addiction Fears Allayed
The patient with sickle cell disease is no more or less prone to addiction to narcotics than any other patient. Despite patients needing large doses of analgesics during a sickle cell pain crisis, studies have shown that they are not actually more likely to develop dependency and addiction, contrary to popular belief.
In fact, a large number of children are undertreated for their sickle cell pain because clinicians fear that these patients will develop addiction.
A survey3 of health care workers treating patients with sickle cell pain, as well as other pain, found that physicians and nurses perceived a much higher percentage of addiction than actually existed.
Pseudoaddictive Behavior
Undertreating pain because of fear of addiction predisposes patients to the development of pseudoaddictive behavior. This behavior is characterized by children with sickle disease seeking and hoarding drugs due to fear of pain and usually disappears when pain is adequately managed.
Despite many health care workers' perceptions, the frequency of drug addiction in patients with sickle cell disease4 is only 1 to 3 percent.
How to Avoid Addiction
 Within these small percentages of young patients who do become hooked on pain medications, dependency and addiction problems are caused by:
Within these small percentages of young patients who do become hooked on pain medications, dependency and addiction problems are caused by:
- inappropriate treatment of any pain with strong opiates
- abuse of pain medication by taking opiates for non-pain-related problems
Patients and parents must be educated to learn to evaluate the type and level of pain and use a stepwise approach to management. For example, Ibuprofen should be used for minimal to moderate pain whereas opioids should be used to severe pain. The dose of each medication should be started at the lowest dose possible and increase according to the child’s pain scale.
Watching Medications
Non-opiate analgesics, such as ibuprofen, should be used for the common pains of headaches, muscle and joint pains, chronic pain, and menstrual pain. Learn about psychoactive substance abuse.
Alcohol and cocaine must be avoided in these children because of their tendency to regularly precipitate pain episodes and more serious complications in sickle cell disease.
Many patients get into trouble because they start taking their pain medications for the mood altering potential. Avoid the use of pain medications for stress, sleep, anxiety, or to prevent pain episodes.
Getting the Right Help
 Sickle cell disease is heartbreaking to see because it affects children with such excruciating pain, but if the treatment is managed correctly, their pain could resolve within a day or two.
Sickle cell disease is heartbreaking to see because it affects children with such excruciating pain, but if the treatment is managed correctly, their pain could resolve within a day or two.
After several pain crises, children become aware of their typical pain pattern and are usually able to verbalize which treatments works best. Take a step back and listen to these kids as they become experts on their pain, and remember that their chance of addiction to pain medications is low.
Community Discussion – Share your thoughts here!
Have you had experience with Sickle cell disease, what advice do you have to share?
About the Author:
Rachael Mattice is the Content Manager for Sovereign Health Group, an addiction, mental health and dual diagnosis treatment provider. Rachael is a creative and versatile journalist and digital marketing specialist with an extensive writing and editing background.
Her portfolio includes numerous quality articles on various topics published in print and digital formats at award-winning publications and websites.
To learn more about Sovereign Health Group’s mental health treatment programs and read patient reviews, visit http://www.sovhealth.com/. Follow Sovereign Health Group on Twitter, Facebook, Google+ and LinkedIn.
The opinions and views of our guest contributors are shared to provide a broad perspective of addiction. These are not necessarily the views of Addiction Hope, but an effort to offer discussion of various issues by different concerned individuals.
Resources:
- Sickle Cell Disease Data & Statistics. (n.d.). Retrieved April 27, 2015, from http://www.cdc.gov/ncbddd/sicklecell/data.html
- Sickle Cell Disease Research & Care. (2012, April 1). Retrieved April 27, 2015, from https://www.nhlbi.nih.gov/news/spotlight/fact-sheet/sickle-cell-disease-research-care
- Health professional perceptions of opioid dependence among patients with pain. (1995, September 1). Retrieved April 27, 2015, from http://www.ncbi.nlm.nih.gov/pubmed/7662056
- Approach to the Vaso-occlusive Crisis in Adults with Sickle Cell Disease. (2000, January 1). Retrieved April 27, 2015, from http://www.aafp.org/afp/2000/0301/p1349.html
Last Updated & Reviewed By: Jacquelyn Ekern, MS, LPC on May 6th, 2015
Published on AddictionHope.com
