 Contributor: Rachael Mattice is the Content Manager for Sovereign Health Group, an addiction, mental health and dual diagnosis treatment provider. Rachael received her bachelor’s degree in journalism and mass communication from Purdue University.
Contributor: Rachael Mattice is the Content Manager for Sovereign Health Group, an addiction, mental health and dual diagnosis treatment provider. Rachael received her bachelor’s degree in journalism and mass communication from Purdue University.
Joint replacement represents a significant advance in the treatment of painful and disabling joint diseases. These surgeries can be done on any joint in the body including the knee, hip, shoulder, foot, elbow, wrist and fingers. Among these procedures, hip and knee total joint replacements are by far the most common.
Climbing Numbers
A new study presented at the American Academy of Orthopaedic Surgeons in New Orleans on March 11, 2014, has shed light on the number of Americans who are living with artificial knees or hips: More than 7 million people in the United States have had knee or hip replacement surgeries, 4.7 million knee replacements and 2.5 million hip replacements.
About 1 million new total knee and hip replacements are performed in the U.S. every year, and that number is expected to grow. There are 1.5 times as many people who have had a joint replacement in America as people who have had heart failure at any one given time, according to Orthopedic Network News. Common indications for joint replacement surgery include osteoarthritis, osteoporosis and joint injuries.
Pain’s Impact on Recovery
Joint replacement is a major surgery that requires weeks to months of physical rehabilitation. Pain medication is a very important adjunct therapy in the recovery period for joint replacement surgery.
Intravenous narcotic (opioid) pain medication, such as morphine, hydromorphone and fentanyl, are given to patients around the clock in the hospital after surgery, and these patients are sent home with a large supply of oral narcotics to alleviate the pain.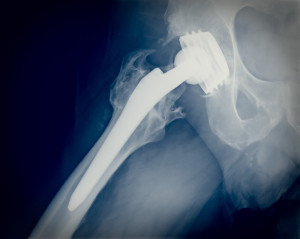 Common oral narcotics that patients are sent home with include Percocet, Lortab and Tylenol with codeine.
Common oral narcotics that patients are sent home with include Percocet, Lortab and Tylenol with codeine.
Pain Medications
The physical pain after a joint replacement is severe and pain medications are absolutely needed. When patients are recovering from joint replacement, intense pain interferes with physical therapy, which can slow down the healing process and recovery phase, not to mention cause anguish for the patient. Patients often refuse to walk after surgery because they are afraid to be in a state of pain.
Unfortunately, narcotics are addictive, and some patients can be led down a dark pathway to addiction. The majority, 95 percent, of patients who undergo a joint replacement do relatively well and do not become addicted to narcotics. However, a small population, approximately 5 percent, of patients do get hooked on pain medication.
Who is Prone to Narcotic Addiction?
People who continue to use narcotics months after joint replacement surgeries, do so because of non-pain related factors, such as emotional stress, addiction, depression and the previous use of narcotic pain medications. Those with symptoms of depression had a 42 percent increased risk of narcotic addiction compared to those who did not have depressive symptoms.
The evidence shows that physical pain is not a reason why these individuals get hooked on narcotics. Patients who were using opioids (narcotics) for pain relief before their procedure, whether prescribed or not, had a 73 percent increased chance of using the drugs after their surgery . These patients also require a higher dose of narcotics to maintain the same effect because they have built up a tolerance to that drug.
Withdrawal Symptoms
Patients who take opioids for a duration of 30 days or longer will develop opioid dependence, which will cause withdrawal symptoms if the pain medication is abruptly stopped. Patients who have physical dependence are not necessarily addicts.
Physical dependence refers to the body’s physical changes as a result of the drug, such as withdrawal symptoms upon cessation of the drug. Addiction is the compulsive use of drugs for non-medical indications. Addiction is considered a behavior,  because these addicted patients are unable to psychologically cope without these medications.
because these addicted patients are unable to psychologically cope without these medications.
Negative Effects Of Opioid Use Before Surgery
In the Nov. 2, 2011, Journal of Bone & Joint Surgery, a study by Michael Mont M.D., and colleagues showed that patients who used opioids before their joint replacement surgery had longer hospital stays, more postoperative pain, and higher complication rates than those who were not opioid dependent.
They were also more likely to need additional procedures, require referrals for pain management, suffer from unexplained pain or stiffness, and have lower function and less motion in the replaced joint. Common opioid side effects include nausea, confusion, constipation and sedation, all of which can interfere with recovery after any type of surgery.
Non-narcotic Alternatives
A study in the September 2007 issue of Clinical Anesthesiology, showed that gabapentin, commonly referred to as Neurontin, a medication often used for seizures and neuropathic pain, has proven beneficial in patients who underwent a total knee or hip replacement.
This study showed that patients who were prescribed gabapentin before surgery required less opioid therapy in the acute phase of recovery. Patients receiving gabapentin postoperatively used significantly less intravenous morphine at 24 hours after surgery.
Alternative Medications
 Nerve blocks, acetaminophen (Tylenol) and nonsteroidal anti-inflammatory drugs (NSAIDs), such as ibuprofen (Advil), are alternative non-narcotic pain medications that can be used preoperatively and postoperatively in intravenous and oral form to relieve pain and decrease the use of opioids in these patients.
Nerve blocks, acetaminophen (Tylenol) and nonsteroidal anti-inflammatory drugs (NSAIDs), such as ibuprofen (Advil), are alternative non-narcotic pain medications that can be used preoperatively and postoperatively in intravenous and oral form to relieve pain and decrease the use of opioids in these patients.
There’s a delicate balance between pain relief and narcotic use. It is important that physicians and patients discuss pain management before the surgery as well as after the surgery so a plan is in place. Many physicians will have patients sign a pain contract indicating that they will become opioid independent after a certain amount of weeks after a surgery.
If you or somebody you know is addicted or dependent on narcotics, there are many drug rehabilitation centers and programs that can assist patients in becoming opioid free.
Community Discussion – Share your thoughts here!
Have you or someone you loved had joint replacement surgery? Did you or your loved one use natural ways to relieve the pain during recovery? What advice do you have to share?
About the Author:
Rachael Mattice is the Content Manager for Sovereign Health Group, an addiction, mental health and dual diagnosis treatment provider. Rachael is a creative and versatile journalist and digital marketing specialist with an extensive writing and editing background.
Her portfolio includes numerous quality articles on various topics published in print and digital formats at award-winning publications and websites. To learn more about Sovereign Health Group’s mental health treatment programs and read patient reviews, visit http://www.sovhealth.com/. Follow Sovereign Health Group on Twitter, Facebook, Google+ and LinkedIn.
The opinions and views of our guest contributors are shared to provide a broad perspective of addiction. These are not necessarily the views of Addiction Hope, but an effort to offer discussion of various issues by different concerned individuals.
Last Updated & Reviewed By: Jacquelyn Ekern, MS, LPC on May 6th, 2015
Published on AddictionHope.com
